- Dental implants in Turkey use the same premium systems (Straumann SLActive, Nobel Active, Osstem TS III, MIS C1, Medentika) found in London, New York and Sydney — at 65–80% lower cost.
- A single Straumann SLActive implant with zirconia crown costs €650–€900 in Antalya, compared to £2,800–£4,200 in the UK, $3,500–$6,000 in the US, or AU$5,500–AU$7,500 in Australia.
- Peer-reviewed 10-year survival data: Straumann 97.2%, Nobel Biocare 96.4%, Osstem 94.8%, MIS 93.1%, Medentika 92.5% (Chrcanovic 2018; Howe 2019; Moraschini 2015).
- Advanced bone augmentation (sinus lift, GBR, onlay grafts, zygoma) allows implant placement even in severely atrophic jaws — 96% success when performed by an experienced surgeon.
- The 2026 digital workflow — CBCT-guided surgery, intraoral scanning, same-day provisional loading — reduces chair time by 40% and places implants within 0.3 mm of planned position.
- Peri-implantitis is the #1 long-term risk; disciplined home care and 6-month professional maintenance reduce incidence from 22% to under 6% at 10 years (Berglundh et al., 2018).
- Stom Dental Centre offers a 10-year clinical warranty on every implant placed, backed by Dr. Telman Iskender and a full implantology team.
- Most cases complete in 2 trips to Antalya over 3–6 months; immediate loading protocols deliver fixed teeth in 72 hours when biology permits.
Choosing dental implants in Turkey in 2026 is no longer a question of whether the quality is comparable to the UK, Germany, or the US — the peer-reviewed data is clear that it is — but which implant system, which surgical protocol, and which clinic best fits the patient in front of the mirror. This 2026 complete guide to dental implants Turkey focuses on the engineering differences between Straumann SLActive, Nobel Active, Osstem TS III, MIS C1 and Medentika; on the bone augmentation techniques that make implants possible even after decades of edentulism; on ten-year survival data from Chrcanovic, Esposito, Buser and Albrektsson; and on the 2026 digital workflow that makes guided, predictable implant placement the new standard of care. Whether you are replacing one tooth or considering a full-arch All-on-6 rehabilitation, the decisions made before surgery — implant brand, surface chemistry, bone preparation, loading protocol — will determine whether your implant lasts 8 years or 30. Stom Dental Centre, Antalya, under the direction of Dr. Telman Iskender, has placed over 12,000 implants across five premium systems since 2009, and this guide distils that clinical experience into the information a patient actually needs.
What a Dental Implant Actually Is — Osseointegration Explained
A modern dental implant is a three-component system designed to replicate a natural tooth root-to-crown unit: the fixture (titanium screw placed into the jawbone), the abutment (connector rising through the gum), and the prosthetic crown (the visible tooth, usually zirconia or lithium disilicate). The fixture is typically 3.3–5.0 mm wide and 8–14 mm long, machined from commercially pure titanium Grade 4 or titanium-zirconium (Roxolid) alloy.
What makes an implant succeed is osseointegration — a term coined by Per-Ingvar Brånemark in 1965 after he observed that rabbit femur bone formed a direct structural and functional connection with titanium without fibrous tissue in between. In humans, osseointegration occurs over 6–16 weeks depending on bone density, surface chemistry and loading conditions. The titanium oxide layer (TiO₂) on the implant surface interacts with osteoblasts, which deposit new bone in direct contact with the fixture. When complete, the implant is biomechanically indistinguishable from a natural tooth root.
Three factors determine whether osseointegration succeeds:
- Surface technology — Sandblasted Large-grit Acid-etched (SLA), SLActive (hydrophilic), TiUnite (anodised), CA (calcium-coated), BLB (blasted). Hydrophilic surfaces cut integration time from 12 to 6 weeks.
- Primary stability at placement — measured in Ncm of insertion torque. Below 20 Ncm, the implant micro-moves under load and fibrous tissue forms instead of bone. Above 35 Ncm, immediate loading becomes possible.
- Host biology — uncontrolled diabetes, smoking >10 cigarettes/day, untreated periodontitis and certain medications (bisphosphonates, high-dose steroids) reduce integration success by 8–25%.
Implant System Comparison — Straumann vs Nobel vs Osstem vs MIS vs Medentika
The single most common patient question in 2026 is: “Which implant brand are you using?” The honest answer is that no single system is “best” for every case — each has engineering strengths matched to specific clinical situations. Below is the component matrix we use at Stom Dental Centre when matching system to patient.
| System | Origin | Surface Tech | Warranty | Best Use | Price (TR) |
|---|---|---|---|---|---|
| Straumann BLX / SLActive | Switzerland | SLActive hydrophilic, Roxolid (Ti-Zr) | Lifetime (mfr.) | Soft bone, immediate loading, medically compromised | €750–€900 |
| Nobel Active / NobelParallel | Sweden / USA | TiUnite anodised, hybrid threading | Lifetime (mfr.) | Fresh extraction sockets, soft bone, All-on-4 | €700–€850 |
| Osstem TS III / TS IV | South Korea | SA (sandblasted & acid-etched), CA calcium-coated | Lifetime (mfr.) | Dense D1–D2 bone, single restorations, full-arch | €500–€650 |
| MIS C1 / V3 | Israel / Germany (Dentsply) | B+ sandblasted dual-thermo-etched | Lifetime (mfr.) | Aesthetic zone, platform-switched sites, triangular V3 for thin ridges | €450–€600 |
| Medentika (Straumann Group) | Germany | Microstructured sandblasted/etched | 10 years (mfr.) | Budget-conscious, standard cases, single tooth gaps | €400–€550 |
At Stom Dental Centre we hold surgical stock of all five systems and provide the manufacturer’s implant passport (lot number, reference, placement date) with every case — a document your home dentist can use for any future maintenance, anywhere in the world.
2026 Cost Comparison — UK, Germany, Switzerland, US & Antalya
Below are current 2026 market prices for the most common implant cases, all-inclusive (implant + abutment + crown + CBCT + surgery + first follow-up). Prices for complex cases assume 4 implants for All-on-4, 6 for All-on-6 and 12 for full-mouth (6 per arch).
| Case | UK (£) | Germany (€) | Switzerland (CHF) | USA ($) | Antalya (€) |
|---|---|---|---|---|---|
| Single implant + crown | £2,800–£4,200 | €2,400–€3,500 | CHF 4,500–6,000 | $3,500–$6,000 | €400–€900 |
| 3-unit implant bridge | £6,500–£9,500 | €5,800–€8,500 | CHF 10,000–14,000 | $8,500–$13,000 | €1,400–€2,200 |
| All-on-4 (per jaw) | £14,000–£22,000 | €12,000–€18,000 | CHF 22,000–32,000 | $18,000–$30,000 | €3,800–€6,000 |
| All-on-6 (per jaw) | £17,000–£26,000 | €14,000–€22,000 | CHF 26,000–38,000 | $22,000–$35,000 | €4,800–€7,000 |
| Full-mouth (12 implants) | £32,000–£48,000 | €28,000–€42,000 | CHF 52,000–75,000 | $42,000–$65,000 | €9,500–€14,000 |
Savings vs. Switzerland: ~€28,000 per jaw — covers travel, hotel and a Mediterranean holiday several times over.
Bone Augmentation Protocols — When the Jaw Isn’t Ready
Perhaps 35–40% of patients seeking implants, especially after years of edentulism, arrive with insufficient bone volume for standard placement. Modern augmentation protocols — refined over 30 years by Buser, Urban, Chiapasco and others — mean that almost no patient is truly “not a candidate.” The right technique depends on the direction and magnitude of bone loss.
For atrophic upper posterior jaw where the sinus has pneumatised. Lateral window (Tatum/Boyne technique) when <4 mm residual bone; crestal (Summers) when 5–8 mm. Xenograft (Bio-Oss) + collagen membrane.
Healing: 6–9 months before loading. Success: 94–97%.
For horizontal and small vertical defects. Titanium-reinforced PTFE or resorbable collagen membrane with particulate xenograft, often combined with implant placement (simultaneous GBR) when primary stability allows.
Healing: 4–6 months. Success: 92–96%.
For significant horizontal or vertical loss (>4 mm). Autogenous block from ramus or chin, or allogenic block. Fixed with osteosynthesis screws; implant placed in second surgery.
Healing: 5–7 months. Success: 88–93%.
For severe maxillary atrophy where sinus lift is inadequate. 30–55 mm implants anchored in the zygomatic bone. Often loaded immediately with fixed provisional. Reserved for experienced surgeons.
Healing: immediate load. Success: 95–98% (Aparicio 2014).
The 5-Phase Clinical Timeline
A predictable dental implant result in 2026 follows a five-phase protocol. The timeline below is what a patient treated at Stom Dental Centre actually experiences — digital from end to end.
The 5-Phase Dental Implant Protocol
Consultation + CBCT
- Online case review
- 3D CBCT scan
- Intraoral digital scan (Medit/3Shape)
- Guided surgery planning
- Written treatment plan
Extraction + Graft
- Atraumatic extractions
- Socket preservation
- Sinus lift / GBR if required
- Bio-Oss + membrane
- Primary soft-tissue closure
Implant Placement
- Guided surgery with stent
- Straumann / Nobel / Osstem
- ISQ stability measurement
- Immediate provisional if torque >35 Ncm
- Post-op protocol
Healing (home)
- Osseointegration
- Soft-tissue maturation
- Wear provisional
- Monthly WhatsApp review
- Photo check-ins
Final Prosthetic
- Final intraoral scan
- Zirconia crown fabrication
- Try-in + bite adjustment
- Screw-retained placement
- Occlusal calibration
Which Implant System for Which Patient? — The Decision Matrix
No single implant system excels in every clinical situation. The decision matrix below reflects how we match system to patient at Stom Dental Centre, based on bone biology, lifestyle factors and aesthetic demands.
45 y/o male, severe grinding, posterior tooth loss
Recommended: Straumann BLX / Osstem TS III, wide-platform (5.0 mm), splinted bridge.
Bruxism doubles axial load. Wide implants, cross-arch splinting and a protective night guard are non-negotiable. Avoid narrow 3.3 mm implants in load-bearing posterior sites.
52 y/o, 15 cigarettes/day, wants full-arch restoration
Recommended: Straumann SLActive (hydrophilic) — fastest integration, lowest failure in compromised healing.
Smoking doubles peri-implantitis risk (Strietzel 2007). Hydrophilic surface halves integration time. Patient counselling on cessation and 3-month recall are essential.
28 y/o female, single anterior implant, high smile line
Recommended: Nobel Active or MIS V3 — platform-switched, immediate placement & provisional.
Aesthetic zone success depends on preserving buccal bone and papilla. Triangular V3 cross-section or aggressive thread design (Nobel Active) maximises primary stability in extraction sockets.
65 y/o, controlled diabetes (HbA1c 7.2), osteoporosis on bisphosphonates (low-dose oral)
Recommended: Straumann SLActive with Roxolid (Ti-Zr) — highest evidence base in compromised patients.
SLActive reduces integration time from 6–8 weeks to 3–4, minimising micromotion exposure. Pre-op HbA1c optimisation, antibiotic prophylaxis and drug holiday if indicated.
Request your personal implant plan
Every case is reviewed personally by Dr. Telman Iskender and our implantology team. You receive a written surgical plan, system recommendation, fixed price and timeline — free, no obligation.
10-Year Peer-Reviewed Survival Data by System
Implant survival at 10 years is the single most important long-term metric, and the peer-reviewed literature (Chrcanovic 2018 meta-analysis; Howe 2019; Moraschini 2015; Jemt 2019) gives us brand-specific numbers. “Survival” means the implant is still in function; “success” adds criteria for absence of peri-implant bone loss, infection and mobility.
10-Year Implant Survival by System
Sources: Chrcanovic et al. (2018) meta-analysis; Howe et al. (2019) CORR; Moraschini et al. (2015) IJOMS; Jemt (2019) CIDRR.
Two important nuances: first, 10-year survival does not guarantee perfect peri-implant bone levels — the success rate (no bone loss >2 mm, no inflammation) is typically 8–12 percentage points lower than survival. Second, these numbers come from prospective studies with trained surgeons. Survival in everyday practice runs 2–4 points lower. Choosing a clinic with documented volume (we place 1,200+ implants per year at Stom Dental Centre) narrows that gap.
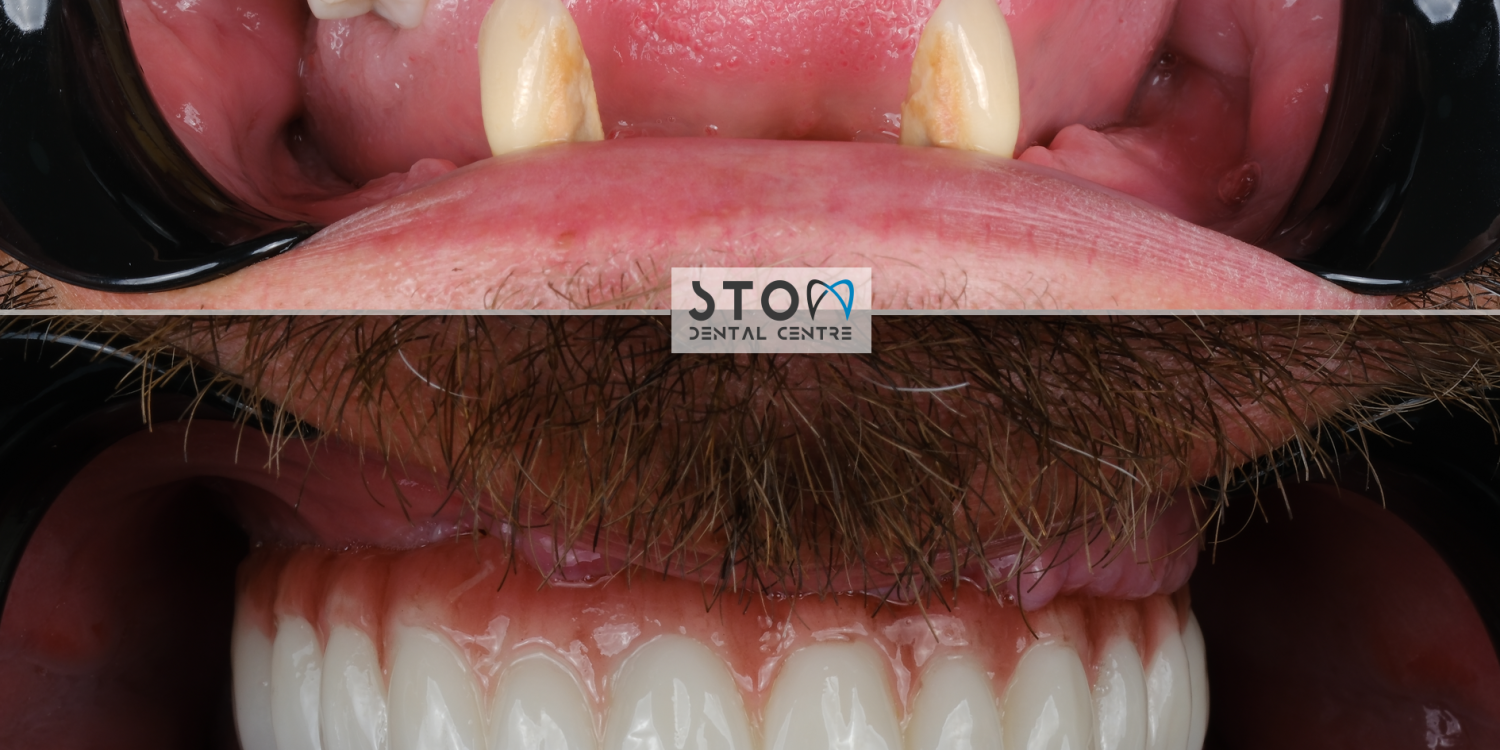
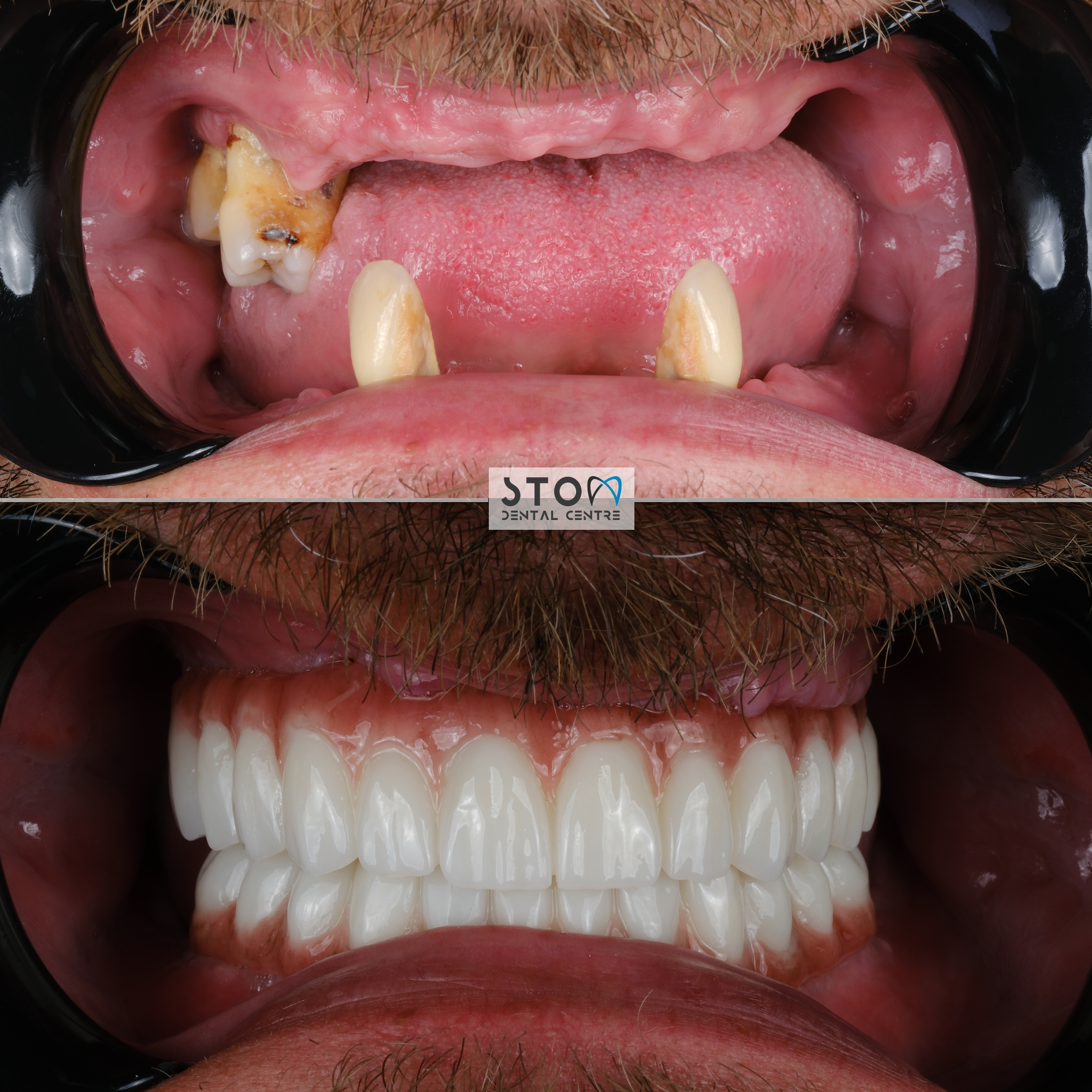
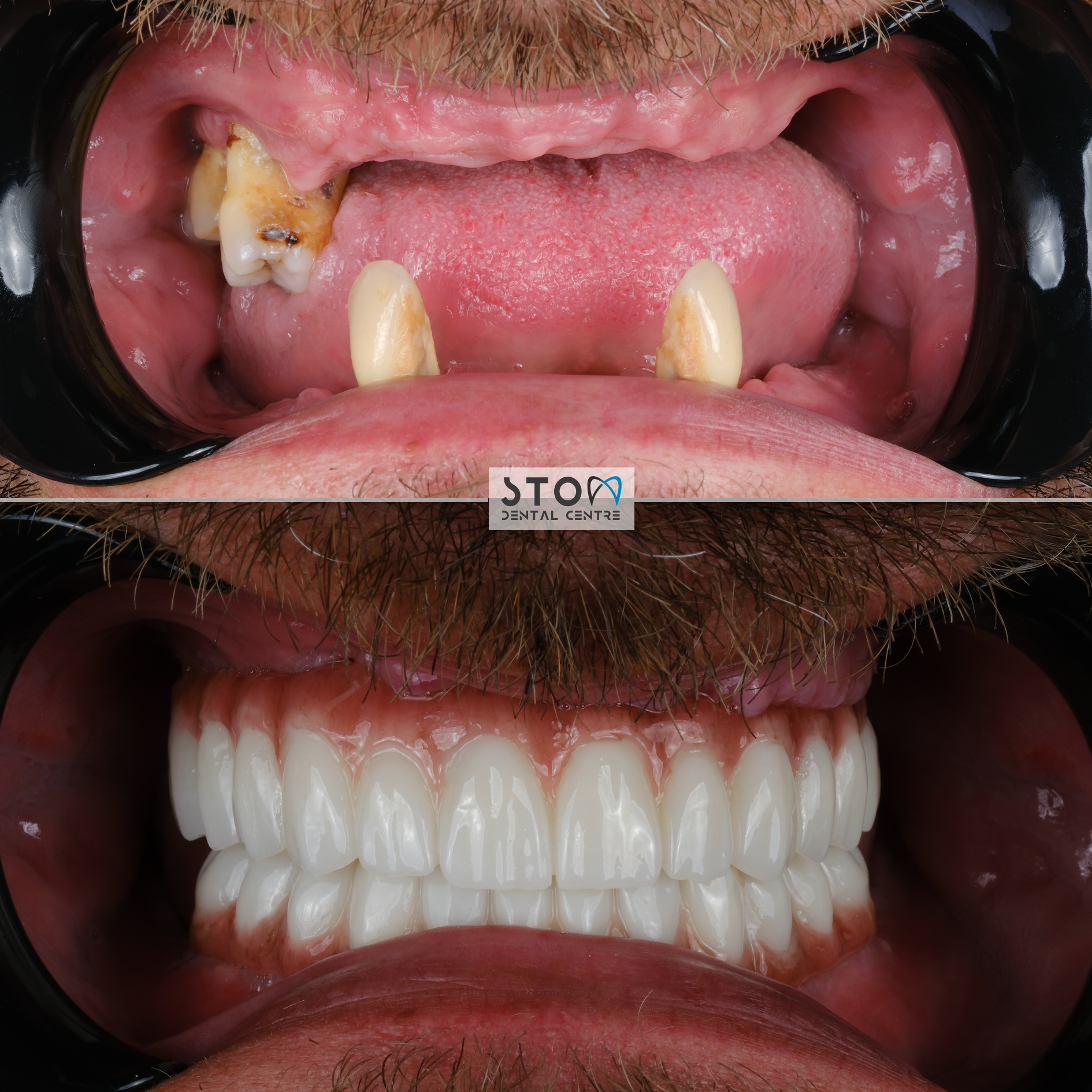
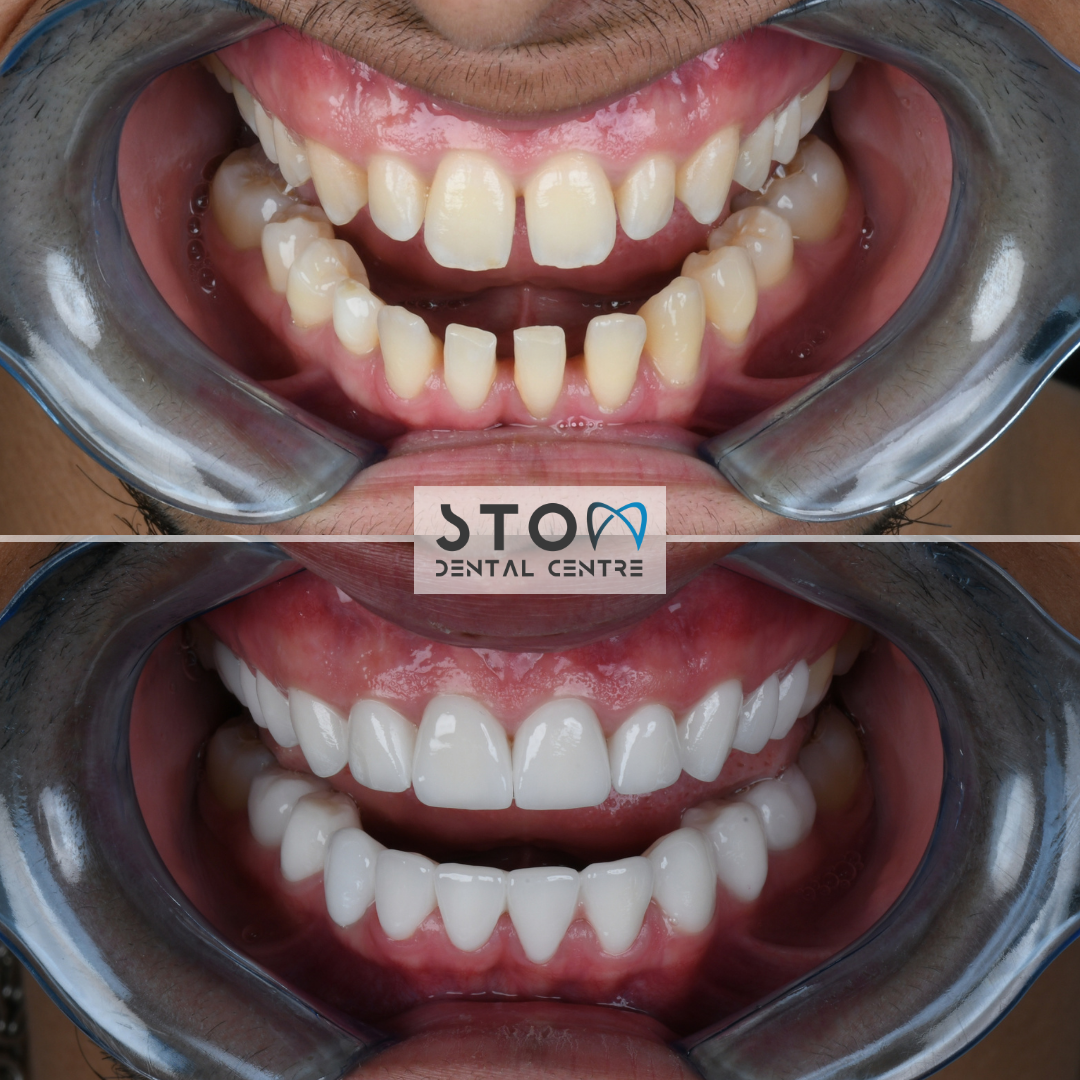
Patient Story — Robert, 58, from London (All-on-6, Three-Year Follow-Up)
Robert, a retired civil engineer from West London, first contacted us in early 2023. He had spent two decades in escalating dental decline — a single failing root canal in his thirties had triggered a cascade of crowns, bridges, and eventually mobile teeth after advancing periodontitis in his early fifties. By 58 he had eight teeth remaining in the upper jaw, all mobile, and a lower arch patched with a 14-year-old precision-attachment partial denture that was now cutting into his gum. His London prosthodontist had quoted £38,400 for an upper All-on-6 and a new lower bridge on existing teeth.
“What changed my mind,” Robert says, “wasn’t the price — although saving twenty-five thousand pounds is not nothing. It was the planning video. Dr. Telman sent me a six-minute video walking through my CBCT scan, showing exactly where each implant would go, how the angle would avoid the sinus on my right side, and what the final bite would look like. I’d seen two specialists in London, and neither had shown me anything like that. It took the fear out of the whole thing.”
Robert’s treatment plan was technically complex. His upper jaw had lost significant bone vertically in the posterior sextants; a bilateral sinus lift using Bio-Oss with collagen membrane was required six months before implant placement. For the fixtures themselves we selected Straumann BLX SLActive (4.5 mm × 12 mm anterior, 4.5 mm × 10 mm posterior) — the hydrophilic surface was chosen specifically because Robert is a former pack-a-day smoker (quit three years before surgery, but the bone vascularity had not fully recovered). Six implants were placed in the upper jaw under full-guided surgery with a 3D-printed surgical stent. On the lower jaw, two Straumann BLX implants were placed in positions 36 and 46 to support a full-arch fixed bridge with his remaining natural teeth.
Phase 2 — 72 hours after implant surgery, with stability measurements confirming ISQ values above 70 on all fixtures, a screw-retained acrylic provisional was fitted in the upper jaw. Robert flew home six days after surgery with fixed teeth — no removable denture, no embarrassment, full speech and a soft diet. Over the following four months he reported by WhatsApp weekly: mild tenderness for ten days, full resolution by three weeks, complete comfort from month two onward.
Phase 3 — Robert returned to Antalya five months after surgery. Intraoral scans were taken, a full-arch monolithic zirconia bridge (Prettau 3 generation) was milled in-house, tried in over two appointments, and screw-retained onto the implants. The bite was calibrated with T-Scan digital occlusal analysis. Total trip 2: five days.
Three years later, Robert returned for his annual review in March 2026. Findings: all eight implants clinically stable, ISQ values between 72–78 (baseline was 70–76 — bone has matured), probing depths 2–3 mm throughout, no bleeding on probing, peri-implant bone levels stable at -0.4 mm from the implant platform (well within the <0.2 mm/year acceptable threshold). Robert's words: “I eat whatever I want. Steak, apples, almonds. I have not thought about my teeth in two years, which is the single best thing I can say about them. My wife says I smile more. I think I’m a better husband for it, actually.” Total cost paid: £13,200. Savings vs. London quote: £25,200.
Peri-Implantitis Prevention — The Eight Rules
Peri-implantitis — inflammation around an implant leading to progressive bone loss — affects 22% of implants by year 10 in unmaintained patients (Berglundh et al., 2018 systematic review). With disciplined care, that number drops below 6%. The eight rules below come directly from the EFP (European Federation of Periodontology) 2022 Treatment Guideline:
- Brush twice daily with a soft manual or oscillating-rotating electric brush — firm brushes damage peri-implant soft tissue. Interdental brushes (0.7–1.1 mm) daily, particularly around screw-retained restorations.
- Single-tufted brush around each implant — reaches the implant neck where plaque initiates peri-implant mucositis.
- Water flosser once daily — superior to string floss around abutments, especially under All-on-4/6 bridges. Waterpik Ultra at medium pressure.
- Professional hygiene every 6 months — or every 3 months if you smoke, have diabetes, or history of periodontitis. Plastic/titanium scalers only, never stainless steel on the implant surface.
- Annual panoramic X-ray or peri-apical series — to catch bone changes before they become clinical. Your home dentist can do this and send us the file for remote review.
- Wear your night guard every night — occlusal overload is the second-biggest cause of peri-implant bone loss after infection. Non-negotiable for bruxers.
- Stop smoking — or cut to under 10 cigarettes/day. Smoking doubles peri-implantitis risk and halves response to treatment if it develops.
- Control systemic disease — HbA1c under 7.5 if diabetic, vitamin D above 30 ng/mL, no uncontrolled GERD. Peri-implant tissues are an accurate mirror of systemic health.
“People ask me which implant is best. The honest answer is that the implant is only 40% of the outcome. The other 60% is the surgical protocol — is the bone prepared correctly, is the soft tissue managed, is the position driven by the planned crown — and the patient’s long-term discipline. A Straumann placed carelessly will fail faster than a Medentika placed beautifully. At Stom Dental Centre we treat every implant as if it were going into my own mouth. That’s why we plan in 3D before we touch a bone, why we photograph every stage, and why our ten-year warranty is credible rather than marketing.”
Most patients consider implants for months before reaching out. That’s exactly the right pace. When you’re ready, we’re here to listen — no pressure, no sales calls. Send your X-ray and a few photos, and we’ll give you an honest specialist opinion. Many patients learn they need less than they feared.
Frequently Asked Questions
Which implant brand is actually the best in 2026?
No single brand is universally “best.” For compromised healing (smoker, diabetic, soft bone) the peer-reviewed evidence base favours Straumann SLActive. For fresh extraction sockets and immediate placement, Nobel Active’s aggressive threading produces excellent primary stability. For dense bone and budget-conscious patients without compromising longevity, Osstem TS III delivers 10-year survival within one percentage point of Straumann. At Stom Dental Centre we stock all five major systems and match system to patient rather than forcing every case into one brand.
How much do dental implants cost in Turkey in 2026?
A single implant with zirconia crown at Stom Dental Centre ranges from €400 (Medentika) to €900 (Straumann SLActive), all-inclusive of CBCT, surgery, abutment, crown and first follow-up. Full-arch All-on-6 with Straumann runs €6,000–€7,000 per jaw. Full-mouth rehabilitation (12 implants, two arches) is €9,500–€14,000 depending on system and grafting needs. These prices represent a 65–80% saving vs. UK/US/Swiss clinics for identical materials.
Is a Turkish implant the same quality as one placed in London or New York?
Yes — provided you choose an accredited clinic. The physical implant (a Straumann SLActive placed in Antalya) is literally the same product shipped from Basel as the one placed in Harley Street. The lab materials (Prettau zirconia, e.max) are identical. What differs is overhead: clinic rent, staff salaries and insurance in Turkey are a fraction of UK/US equivalents, and that difference passes to the patient. The variable is the surgeon — which is why patient due diligence (peer-reviewed volume, documented cases, CBCT planning) matters more than country.
How long do dental implants last?
Peer-reviewed 10-year survival is 92–97% depending on system. Real-world lifespan, with disciplined maintenance, is 20–30 years for the implant fixture itself and 12–18 years for the crown. At Stom Dental Centre we have patients with implants placed in 2010–2012 still in perfect function in 2026, with crowns on their first or second replacement. The implant is essentially a permanent component; the prosthetic above it is a long-term but replaceable component.
Can I have implants if I’ve been told I don’t have enough bone?
In 2026, “not enough bone” is almost never a final answer. Sinus lift (94–97% success), guided bone regeneration, autogenous block grafts and zygomatic implants between them handle virtually every anatomical situation. Our CBCT-based planning determines the exact augmentation protocol needed. Patients who were told they needed dentures forever routinely leave Stom Dental Centre with fixed teeth.
Is same-day (immediate loading) really safe?
Yes, when biology allows. The All-on-4/6 protocol with immediate provisional loading requires insertion torque >35 Ncm and cross-arch splinting, with a soft diet for 3 months. Peer-reviewed 5-year survival of immediate-loaded All-on-4 is 96.8% (Maló et al., 2019). For single posterior implants under heavy occlusal load, delayed loading (3–6 months) remains our standard.
What is the difference between All-on-4 and All-on-6?
All-on-4 uses four implants per jaw (two anterior vertical, two posterior angulated 30–45°); All-on-6 uses six implants (two anterior, two mid-arch, two posterior). All-on-6 distributes load better, making it preferable for bruxers, heavy chewers, and lower jaws where bone density is higher. All-on-4 remains appropriate for atrophic upper jaws where avoiding sinus lift is a priority. Survival rates are statistically similar at 10 years (All-on-4: 94.8%; All-on-6: 96.1%).
What complications should I be prepared for?
The three main complications at 10-year follow-up are: peri-implantitis (22% untreated, 6% with maintenance) — prevented by the eight rules above; screw loosening in the abutment (5–8%, easily retightened in a 15-minute appointment); and ceramic chipping on the crown (3–7% at 10 years, repaired by crown remake, covered under our warranty). Implant fixture fracture is rare (<0.3%) and typically occurs in bruxers without a night guard.
References & Verifiable Sources
All clinical survival data, surgical protocols and cost comparisons cited in this guide are drawn from peer-reviewed literature and publicly verifiable sources. We encourage independent verification:
- Chrcanovic BR, Kisch J, Albrektsson T, Wennerberg A. “A retrospective study on clinical and radiological outcomes of oral implants in patients followed up for a minimum of 20 years.” Clinical Implant Dentistry and Related Research, 2018 — PubMed
- Esposito M, Grusovin MG, Felice P, Karatzopoulos G, Worthington HV, Coulthard P. “Interventions for replacing missing teeth: horizontal and vertical bone augmentation techniques for dental implant treatment.” Cochrane Database of Systematic Reviews — Cochrane Library
- Buser D, Sennerby L, De Bruyn H. “Modern implant dentistry based on osseointegration: 50 years of progress, current trends and open questions.” Periodontology 2000, 2017 — PubMed
- Berglundh T, Armitage G, Araujo MG, et al. “Peri-implant diseases and conditions: Consensus report of workgroup 4 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions.” Journal of Clinical Periodontology, 2018 — PubMed
- Albrektsson T, Chrcanovic B, Östman PO, Sennerby L. “Initial and long-term crestal bone responses to modern dental implants.” Periodontology 2000, 2017 — PubMed
- Howe MS, Keys W, Richards D. “Long-term (10-year) dental implant survival: A systematic review and sensitivity meta-analysis.” Journal of Dentistry, 2019 — PubMed
- Moraschini V, Poubel LAC, Ferreira VF, Barboza EdSP. “Evaluation of survival and success rates of dental implants reported in longitudinal studies with a follow-up period of at least 10 years.” International Journal of Oral and Maxillofacial Surgery, 2015 — PubMed
- T.C. Sağlık Bakanlığı — Uluslararası Sağlık Turizmi Daire Başkanlığı (Turkish Ministry of Health, International Health Tourism Authority) — shgmturizmdb.saglik.gov.tr
Medical disclaimer: This article is for educational purposes and does not constitute clinical diagnosis. Individual treatment outcomes depend on patient-specific factors. Stom Dental Centre is a licensed private dental clinic registered with the Turkish Ministry of Health (Muratpaşa/Antalya). Our implantology team holds certifications from ITI, DGI and ICOI.